Did you know there are at least twenty different types of contraception available? Here we’ve compiled a list with a brief explanation for each to help you learn about your many options. Ovatures recommends speaking to a licensed Women’s Healthcare professional regarding which type of contraception may be most suitable for you.
1- Barrier contraceptives
- Condoms: there are no contraindications for these. Condoms are the best method for preventing sexually transmitted diseases (STDs)
- Spermicide: this acts as a chemical barrier, preventing sperm from reaching the uterus. It must be used in conjunction with another method because its effectiveness is low when used on its own.
- Female condoms: these are made from nitrile rubber. They protect the user from unwanted pregnancy and from STDs. They are less effective than the male version.
- The diaphragm: a flexible silicone dome that is positioned against the cervix. It does not cover the mucous membrane of the vagina and therefore it is not recommended for avoiding STDs.
- The vaginal sponge: this is a device made from polyurethane foam containing spermicide. It should only be removed after 6 hours have elapsed since having sex. It does not prevent STDs.
2- Hormonal contraceptives
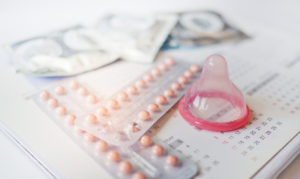 The pill: this should only be taken with a prescription from a doctor. It can help with several problems like irregular or painful periods, but it also may have side effects.
The pill: this should only be taken with a prescription from a doctor. It can help with several problems like irregular or painful periods, but it also may have side effects.- The progestogen-only mini pill: this emerged as a result of the side effects caused by the pill due to estrogens. It has to be taken every day at the same time.
- The morning-after pill (MAP): aka “Emergency contraception” or EC. Due to its high dose of hormones, this should only be administered on an occasional basis and within 72 hours of having sex.
- Intrauterine device (IUD): this is a small implant that is placed in the uterine cavity in clinic. It can last for 3 to 10 years depending on the type. Some release hormones, while others do not. Be sure to talk to your doctor or nurse about this highly effective, long-acting reversible contraceptive – it is becoming a very popular option among young women!
- The contraceptive patch: this is a simple adhesive patch that is applied to the skin and needs to be changed once a week.
- The vaginal ring: this is a ring made of an ethylene-vinyl acetate copolymer that releases estrogen and progesterone. It can be inserted by the woman herself. It lasts for three weeks.
- The contraceptive injection: this has different side effects than the pill, but only needs to be administered every three months. The injection is given in clinic.
- The contraceptive implant: this is highly effective as a contraceptive. A subcutaneous implant of a small plastic tube that releases hormones. It lasts for three years.
3- Permanent contraception
- Vasectomy: a simple surgical procedure for men done in clinic in which the vas deferens, which transport sperm, are tied off.
- Tubal ligation: this is a surgical procedure for women done in the operating room to tie off the Fallopian tubes, which transport the egg. It can be done immediately after childbirth or at any time by a minimally invasive outpatient procedure called laparoscopy.
4- Alternative natural methods
- The rhythm or calendar method: you can track your most fertile days with the help of an app. A woman’s most fertile days depends on her cycle length. The problem is that not all women are regular in their menstruation and, furthermore, that there are days when they are at risk in addition to their fertile days so this is typically not considered a very effective method of birth control.
- Coitus interruptus, or the withdrawal method: this involves withdrawing the penis prior to ejaculation. The problem is that the man may not withdraw in time, and also that pre-seminal fluid contains small amounts of sperm.
- Cervical mucous: a few days before ovulation begins, cervical mucous becomes more elastic. This is one way of discovering our fertile period.
- Breastfeeding: women who are breastfeeding, most often do not ovulate, as prolactin (one of the breast feeding hormones) inhibits this process. It is most effective if it is less than six months since giving birth and if the baby is being fed exclusively on breast milk. However, there are many contributing factors that influence the effectiveness of this and as such these factors should be considered carefully with your doctor or nurse.
Seeking more information from a Women’s Healthcare professional, like your Gynecologist or Nurse Practitioner is always recommended. The right method of contraception is different for each individual situation. The Ovatures Team is always here to help if you need to get hooked up with a local provider to discuss which is best for you!




